Sensory
retraining
This sensory retraining program was created by the Cleveland
Clinic to help your recovery. Be sure to follow the rehabilitation
plan your doctor has recommended for you.
This easy-to-follow guide explains sensory retraining exercises
that your doctor may suggest after breast reconstruction using
the Resensation® surgical technique with Avance® (acellular nerve
allograft–arwx).
What is sensory retraining?
Sensory retraining exercises are used to help improve sensation in multiple areas of the body.1-3 The goal is to help retrain the connection between your brain and body with regular practice.
Navigating recovery
Think of sensory retraining as a road map to help guide your recovery after the Resensation surgical technique. There is no deadline for sensory retraining, and each person’s journey is unique. Your doctor can help if you have any questions. And remember that recovery will take time.4
How does sensory retraining work?
10 minutes, twice a day.
Ask your surgeon if it’s okay to start sensory retraining. If approved, you can perform these suggested exercises twice daily, once in the morning and once at night. All you need is a mirror, a cosmetic brush and an ice cube. Spend a minute or two on each step, carefully noticing any sensations. Remember to look at yourself in the mirror as you go—it’s important to watch as you perform the motions.


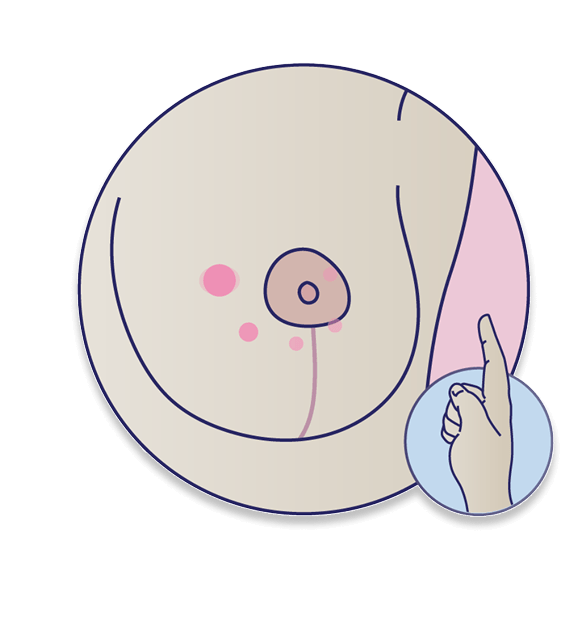
Step 1: Finger taps
Using your pointer finger, softly touch different areas of your breast starting with the nipple (or the center of your breast), and slowly move outward in a clockwise motion. As you move around, tap with the pad of your finger like you would when typing on a keyboard.

Step 2: Finger swirl
Next, repeat the same circular motion from step one. This time, apply continuous pressure as if you’re drawing a swirl on your breast.
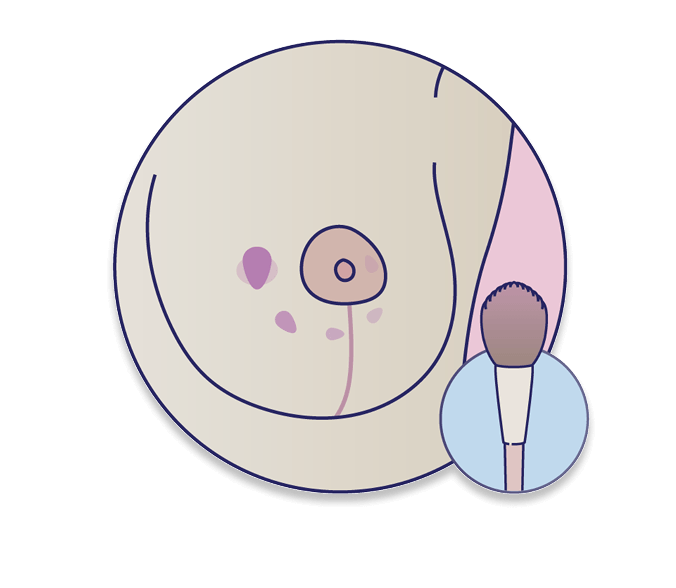
Step 3: Brush taps
Using a soft makeup brush, gently touch different areas of your breast starting with the nipple, and slowly move outward in a clockwise motion.
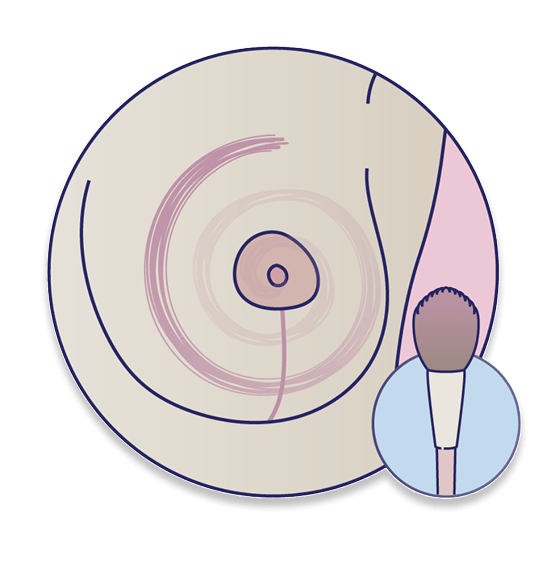
Step 4: Brush trace
With that same brush, trace the area of your breast by applying consistent contact and light pressure. Follow the same clockwise motion, starting with the nipple and moving outward.
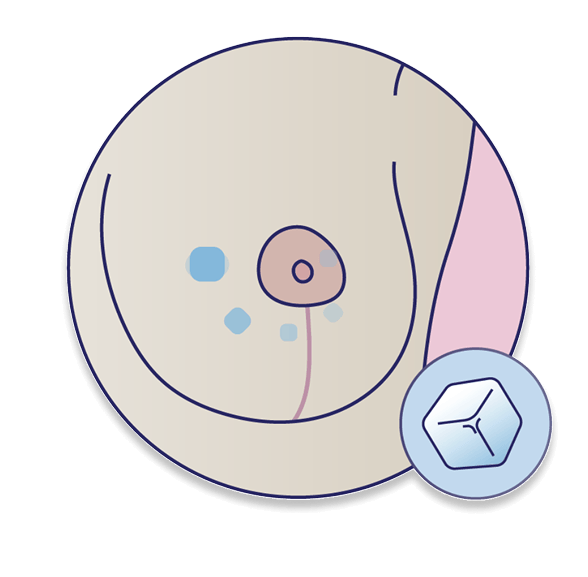
Step 5: Ice touch
Use a cube of ice to touch different areas of your breast starting with the nipple, and slowly move outward in a clockwise motion.

Step 6: Ice trace
Finally, use the ice to trace the same motions you’ve followed from the start.

Step 7: Eyes closed
Once you’ve gone through the flow while watching your movements in the mirror, perform the entire process again with your eyes closed. This time, visualize and imagine yourself performing each step and the connections you’re building between your brain and your repaired nerves.

“No one should have to spend the rest of their life feeling detached from such a fundamental part of who they are.”
-Bri, patient and The Breasties co-founder*
*Individual results may vary based on patient factors and surgical approach. Bri Majsiak was compensated for her time, but the views expressed are her own.
References
- Phillips C, et al. Sensory retraining after orthognathic surgery: effect on patient report of altered sensations. Am J Orthod Dentofacial Orthop. 2009;136(6):788-794. doi:10.1016/j.ajodo.2008.07.015
- Meyer R, et al. Sensory rehabilitation after trigeminal nerve injury or nerve repair. Oral Maxillofac Surg Clin North Am. 2001;13(2):265-376. doi:10.1016/S1042-3699(20)30150-3
- Phillips C, et al. Sensory retraining: a cognitive behavioral therapy for altered sensation. Atlas Oral Maxillofac Surg Clin North Am. 2011;19(1):109-118. doi:10.1016/j.cxom.2010.11.006
- Yano K, et al. Breast reconstruction using the sensate latissimus dorsi musculocutaneous flap. Plast Reconstr Surg. 2002;109(6):1897-1903. doi:10.1097/00006534-200205000-00018
What is AVANCE® (acellular nerve allograft-arwx)?
AVANCE is a sterile nerve graft prepared from donated human tissue. AVANCE is implanted in patients with cut nerves to help restore sensory function.
Important Safety Information
AVANCE has risks related to surgery and the use of donated human tissue that you should understand before treatment.
Surgical and Procedure-Related Risks
As with any nerve repair surgery, complications can occur. Risks related to the surgical procedure and use of AVANCE may include pain, increased sensitivity at the implant site, swelling, bleeding, and infection. Other risks may include scarring (including thick or raised scars), delayed wound healing, scar tissue, and formation of a painful nerve growth. Some patients may experience loss, decrease, or change in sensation or movement in the area being treated. A serious problem involving wound healing has also been reported.
Risk of Infectious Disease Transmission
Because AVANCE is made from donated human tissue, it can pass on infectious diseases. Donors are carefully screened and tested for viruses and other infectious agents. However, these measures do not completely eliminate the risk of disease transmission. All infections thought to be transmitted by AVANCE should be reported to Axogen Corporation at 1-888-296-4361.
What to Watch for After Surgery
After your procedure, your doctor will monitor your healing and nerve recovery. Contact your healthcare provider right away if you notice any of the following:
- Redness, swelling, warmth, or increasing pain at the surgical site
- Drainage or signs of infection
- New or worsening numbness, tingling, or pain
- Changes in movement or weakness
- Any other symptoms that concern you
Always follow your healthcare provider’s instructions during recovery and rehabilitation.

