After a mastectomy, women have multiple breast reconstruction options: implants, free flap reconstruction using natural tissue, or a combination. Each of those techniques has multiple variations.
Despite the differences between the various types of breast reconstruction, all have at least one thing in common.
No matter how great a woman looks after reconstruction, her new breasts will likely be numb. During a mastectomy, the breast tissue is removed and the nerves that supply feeling to the chest are severed. When nerves are severed, nerve signals are disrupted. This usually results in numbness and loss of feeling in the breast area.
Dr. Jules Walters, a board-certified plastic and reconstructive surgeon in New Orleans, Louisiana, was bothered that he couldn’t do more for his patients.
“I would get so excited about my patients’ outcomes in terms of the way they looked, but they’d say, ‘Oh well, I really can’t feel anything,’ or ‘My breasts look great but they’re numb.’ I believe that they just think that’s the way it has to be,” Walters said. “It’s our job as plastic surgeons to educate them and say, ‘This is not how it has to be.’ We can do better for these patients.
To potentially restore sensation to women’s breasts, Walters offers a surgical technique called Resensation to women undergoing breast reconstruction. Resensation uses allograft nerve tissue to reconnect and bridge the gap between the nerves in your chest and the nerves in your reconstructed breast tissue. Over time, this guides regrowth of nerve fibers and can lead to sensory restoration to the breast tissue.
Walters shares why Resensation is an important advancement in post-mastectomy breast reconstruction, what motivated him to incorporate Resensation into his practice and how he thinks Resensation will change what women can expect after breast reconstruction.
Why is it important for women to be made aware that Resensation is a possibility before they undergo mastectomy and breast reconstruction?
Resensation is performed during breast reconstructions. I think it’s so important to get this information to patients as fast as we can once they’re diagnosed with breast cancer because that’s when they must make a lot of decisions very quickly. If they don’t have all of the information, sometimes they’re making these decisions without the appropriate education, which can impact the rest of their life. Just like there are laws now in certain states that say patients must be educated on their reconstructive options, Resensation is something that patients should know about as it may potentially provide them with a better outcome.
What response do you get from patients when you bring up the possibility of Resensation?
Any patient that I talk to about Resensation is definitely interested. But when I first meet with patients, they are often dealing with an active breast cancer diagnosis. They’re in a very anxiety-provoking time in their breast cancer journey.
At that time, they just want the cancer out. It’s a fight-or-flight response. They’re thinking, ‘I need to beat this and I need to survive.’ That’s where it’s my job as a plastic surgeon to listen and let them know that I can not only make them feel whole again, but potentially make their breasts look better than before. And now, we can offer them more than just natural-looking, numb breasts. With Resensation, we can potentially restore sensation.
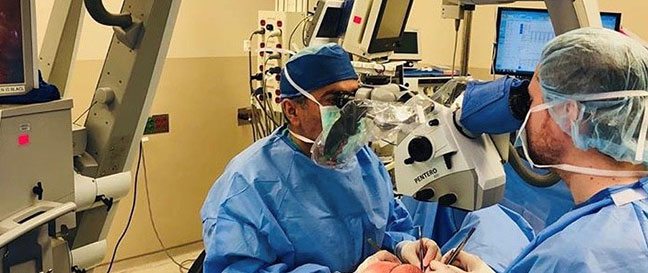
You completed your plastic surgery residency about five years ago. What do you recall being taught at the time about the loss of sensation in the breasts after mastectomy and reconstruction?
I trained in plastic surgery from 2011 to 2014. We talked about size, shape, symmetry and softness, but sensation has been the “silent S” – nobody really talked about it. We never really had a good solution. There were some attempts years ago to do end-to-end nerve repairs – directly connecting the nerve in the chest with the nerve in the flap. But it never worked well because there was too much tension. If a nerve is pulled too tight, it has difficulty growing and the repair may fail.
How does Resensation and the use of Axogen’s Avance Nerve Graft potentially change that?
With the nerve graft, we’re able to bridge the gap between nerves without tension. Tension-free repairs have been key to the success of peripheral nerve repair elsewhere in the body. The allograft acts like a bridge between the newly reconnected nerves to support growth of new nerve fibers and, over time, potentially lead to sensory restoration of the breast tissue.
What did patients tell you about the impact the loss of sensation had on their lives?
For a long time, we’ve focused on making sure the reconstructed breasts look and feel natural to the patient’s partner, while ignoring how it actually feels to the patient.
I had two patients who, after I performed reconstruction, burned their breasts. One was burned on a heating pad. The other had an additional surgery after reconstruction to remove some lymph nodes around her armpit. Post-operatively, she placed an icepack in her armpit to relieve discomfort, fell asleep, and the cold caused an injury to the side of her breast.
I’ve also had patients talk about their insecurities while being intimate with their partners. That’s something patients have been hesitant to talk about, but it does come up. I think the more that we educate and raise awareness, the more patients will then voice their concerns about the impact numb breasts have on their daily life.
What do you hope to be able to offer your patients by incorporating Resensation into breast reconstructions?
I want to offer women the chance to not just have reconstructed breasts, but to be able to look in the mirror and feel beautiful. I want the scars to be minimal, similar to what a woman would have if she had cosmetic surgery. I want them to feel confident and to not be constantly reminded of breast cancer.
With advanced techniques, patients can have those results aesthetically. With Resensation, they can not only look good but potentially have the feeling in their breasts restored.
What does Resensation mean for women facing decisions about mastectomy and breast reconstruction?
Resensation is the next frontier in breast reconstruction. I hope that providing information about this technique that could potentially restore sensation will reduce the fear and anxiety that patients face when they are deciding whether to have a mastectomy or a double mastectomy.
Do you think Resensation will change what women expect from their plastic surgeons when they undergo reconstruction?
It’s going to potentially raise the bar for plastic surgeons who offer breast reconstruction. Plastic surgeons are going to have to learn this technique. This is very meticulous nerve repair. You don’t rush through it. You have to pay attention to detail. But, the possibility to restore sensation is worth it.
About Jules Walters, MD
Certified by the American Board of Plastic Surgery, Dr. Jules Walters specializes in cosmetic surgery of the face, breast and body, as well as breast reconstruction. His academic background includes graduating magna cum laude with a bachelor’s degree in biological sciences from Louisiana State University in Baton Rouge and a medical degree from LSU Medical School in Shreveport. He completed a general surgery residency program at LSU New Orleans, followed by a three-year plastic surgery residency at the University of Texas at Houston. During his residency, Dr. Walters developed a profound interest in breast reconstruction and trained at the Texas Medical Center. Dr. Walters approaches every procedure with an aesthetic sense and believes that dedication to detail is of the utmost importance.
To contact Dr. Walters, visit: www.themodernplasticsurgery.com
_________________________
1https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4408553/
Dr. Walters did not receive compensation from Axogen Corporation for his time in connection with this interview.
Resensation Articles

How does mastectomy impact the nerves in the breast?
One sometimes overlooked aspect of mastectomy is its impact on nerves. Read what happens to nerves during mastectomy and explore…
Read More
What happens during implant breast reconstruction with Resensation®?
By repairing sensory nerves, Resensation® enables you to potentially regain sensation to your chest. Read how this procedure works during…
Read More
how resensation® helped Leanna feel secure in her family’s future
With Resensation®, Leanna can be there to watch her kids grow up—without losing the feeling of being whole.
Read More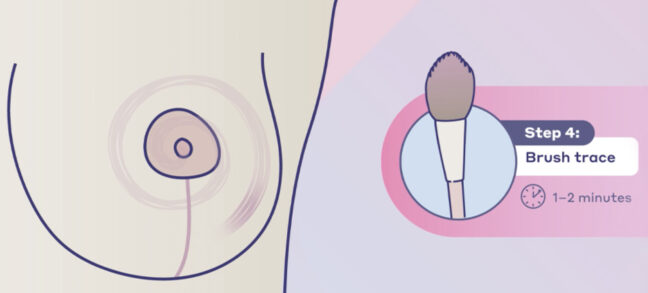
post-surgery sensory retraining: instructions and video guide
Sensory retraining is a series of exercises designed to help you reconnect with your body after breast reconstruction with Resensation®.
Read More