Stephanie lives in a suburb right outside Atlanta with her husband and their three children where she teaches special education.
She loves to spend time with her family, traveling and having fun. If she gets the chance amid the hustle and bustle, she likes to read and work on her vegan cooking skills. Her family has a strong community surrounding them, with Stephanie’s mother and her brother’s family nearby, close friends from work and many neighbors.
With her busy, joyful life, Stephanie didn’t have much time for anything else on her plate. Unfortunately, breast cancer doesn’t take anyone’s schedule into account.
A long path to diagnosis
After Stephanie’s first son was born, back in 2013, she developed a lump in her breast. She went to the doctor, got an ultrasound and was told that it was nothing.
Two years later, her breasts started leaking. She again went to the doctor, had an ultrasound and had some testing done. Again, the results came back negative and Stephanie was told not to worry.
But then in May of 2019, Stephanie’s breasts started leaking again and her OBGYN referred her to a different breast doctor. The new doctor did a mammogram and an ultrasound. “They said the lump didn’t feel like breast cancer, but whatever it was, they were going to take it out, which is not where I was expecting that appointment to go,” Stephanie said.
“So, I go in for the biopsy because there were a couple of places that needed to be checked out. And the surgeon said ‘I’ve seen cancer before. It doesn’t look like a tumor.’ Lo and behold, a week later, he called me and said, ‘Yep, it is cancer cells.’”
Stephanie didn’t know how to respond.
“I actually completely shut down. My husband was like, ‘Well, if you want to talk about it…’ and my mother was more hysterical than I was,” Stephanie said.
“It was, I think, because it was so unexpected. I don’t know if I didn’t process it, if I didn’t want to process it, but it was a complete shut down for a long time,” she said. “Breast cancer doesn’t run in my family, so it was never on my radar. Having to go through other mammograms and ultrasounds for the same thing years prior … for it to go from ‘Oh, it’s nothing’ to then turn out to be something—I was just, I was at a loss for words. I didn’t know what to think or say or feel.”
A plan of attack
Stephanie’s doctor laid out all her options. A lumpectomy. A single mastectomy. A double mastectomy. And she gave Stephanie the technical pros and cons of what each looked like. “She let me know, when surgeons were working, they would test the tumor during surgery to find out if it was invasive, if it spread, and then what would happen if they needed to go from there.”
“I chose to do a single mastectomy. I did not want to do the lumpectomy, because if the tumor turned out to be bigger than what it was, then I wanted to make sure it was all gone [from my breast],” Stephanie said. “But I didn’t want both of my breasts gone. I did all the genetic testing beforehand. And, I just felt like it really wasn’t necessary to do both.”
Stephanie felt strongly about opting for a single, rather than double mastectomy. “I wanted to keep as much of me as possible. I understand being scared, and not wanting cancer to come back. [I understand] wanting to throw the kitchen sink at it, and not wanting to go through this again. But you know, I like my body and I want to keep as much of me as possible, and I thought, ‘I have one good one, so why get rid of it?’”
“It didn’t even register with me that I would not have sensation. That was never … It’s just not something you know to ask about.”
When it came time for her procedure, it was Stephanie’s surgeon who let her know about her options for implants or DIEP flap, and informed her about the opportunity to recover sensation post mastectomy with Resensation.
“To be honest with you, it didn’t even register with me that I would not have sensation. That was never… It’s just not something you know to ask about. And so, if I didn’t have the plastic surgeon that I had, it would not have dawned on me until after I had the surgery. Stephanie said.
Stephanie didn’t know that reconstruction without implants was a possibility. “He explained to me about the fat grafting and the procedure that I got. I didn’t even know that that was an option. When I hear of people having mastectomies, it’s always implants. And so even the procedure [I had] without just the sensation aspect, I was not very familiar with.”
Recovery and recovering a sense of self
Stephanie had her surgery in July of 2019. “I did not go back to work until September, and even when I went back to work in September, I was still not 100%. I was unable to function as my normal self.”
As for regaining sensation, that happened gradually. “I do remember that tingly feeling when the numbness wears off. I started noticing and thinking, ‘Oh man, it’s tingling.’ A feeling like Novocaine wearing off,” Stephanie recalled. “I would say [my sensation] is about 75%. They had to remove my nipple, so around that area I don’t have as much sensation, but the outside of my breast, I definitely have sensation.”
Stephanie is grateful for the sensation she retained in her natural breast, and the sensation she regained in her reconstructed breast.
“A friend of mine went through this before, maybe a year before I did [without Resensation]. One time she was in the pool, and didn’t notice that her swimsuit had come down. I don’t have to worry about that,” she said. “I’m aware of what’s going on with my breast. Like now, bras don’t fit me the same on both my breasts. Bras always rise up on the one side. But I know that it’s riding up. I can feel that my bra is riding up.”
“I’m grateful to have sensation in both breasts”
But it’s not just about clothes. “It’s holding my kids. I had a young one at the time and I was constantly holding him. And intimacy with my husband is a big part of it all, too. Because of Resensation, I can hug my family,” she said.
“I feel my [chest] when I’m embracing someone … I don’t know how I would feel if I put on clothing, if I went to hug my spouse, and I wasn’t able to feel [any of it]. Even just washing up in the shower, you feel the motion. And I don’t know what it would be like to go over a part of my body and feel nothing. That would be very difficult to deal with because you’re already dealing with not looking the same. As well as a doctor can put you back together, it’s never quite the same.”
Resensation allows Stephanie to feel closer to normal. “To have the feeling, to just move throughout my day-to-day. It’s one of those things, you don’t know how bad you miss it until it’s gone. Or you just don’t know how important it was until it’s not there anymore. I’m grateful to have sensation in both [breasts]. And even if it’s not 100%, I know that it’s there. It’s less of a reminder of what has been taken [by cancer].”
Advice for others
Like with any experience in life, there are always things we wish we knew beforehand. For Stephanie, she wishes she had known “the pros and cons from a real-world perspective, not in technical terms. You know, what are the real-life consequences of doing a double or a single mastectomy. If I’m talking to a girlfriend who had it, I definitely learned some pros and cons that a doctor wouldn’t tell me because it’s not technical. It’s more emotional, so those are the things that I wish I would have known before.”
“I would have done it the same way, but, you know, I wish I would have had that info.”
“Cancer has changed me on the inside and on the outside.”
Because of that, Stephanie is happy to share her story, to show the human side of being a breast cancer survivor.
“Do your homework on your surgeon,” she says. “With all the different technologies that are out there, I’m just grateful to have had a team that was up on the latest [solutions]. Because you don’t know what you don’t know. It’s important to be able to have all of that information so you can make the best possible decision for yourself.
The hardest thing Stephanie has had to learn through it all is how to navigate being a new version of herself.
“I’m just not my old self anymore. And that’s very,” she paused, “it’s very difficult. I’m grateful that the cancer is gone. There’s nothing that can beat me being here for my family. But I look in the mirror and … Cancer has changed me on the inside and on the outside.”
“Any way you can get some of your old self back, you should definitely do it. Because cancer takes a piece of you. And I’m just thankful that I can get as much of me back as possible. I do wish for any woman going through this process that they are armed with as much information as possible.”
Some links will navigate you away from the Resensation® website. Links outside of resensation.com are provided as a resource to the viewer, and do not constitute an endorsement or recommendation by Axogen. Axogen accepts no responsibility for or control over the content of the linked sites.
*The level of sensation restored following use of the Resensation technique may vary and cannot be guaranteed, due to unique anatomy and other considerations. Please consult a surgeon for more detailed information.
Each patient outcome is dependent upon the nature and extent of nerve loss or damage, the timing between nerve loss and repair, and the natural course of the patient’s recovery. These testimonials reflect the experience of the particular individual and may not represent typical results.
Resensation Articles

How does mastectomy impact the nerves in the breast?
One sometimes overlooked aspect of mastectomy is its impact on nerves. Read what happens to nerves during mastectomy and explore…
Read More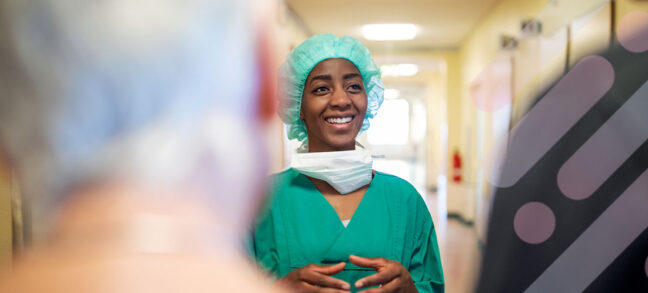
What happens during implant breast reconstruction with Resensation®?
By repairing sensory nerves, Resensation® enables you to potentially regain sensation to your chest. Read how this procedure works during…
Read More
how resensation® helped Leanna feel secure in her family’s future
With Resensation®, Leanna can be there to watch her kids grow up—without losing the feeling of being whole.
Read More
post-surgery sensory retraining: instructions and video guide
Sensory retraining is a series of exercises designed to help you reconnect with your body after breast reconstruction with Resensation®.
Read More