a shock to her system
Ultimately, Jessica was lucky her husband accidentally hit her in his sleep. If it hadn’t been for his tossing—and an errant elbow that landed squarely on her left breast—they might not have discovered the cancer until it was too late.
Because a week after impact, the bruising on Jessica’s breast had turned hard and lumpy to the touch. She knew something wasn’t right, and went to see her OB-GYN. From there, things escalated quickly.
a battle—and a plan
The cancer had been slowly growing in her milk duct, but the trauma of her husband’s elbow caused it to explode out of the duct and into the surrounding breast tissue. A nurse for nearly 20 years, Jessica relied on her knowledge of medicine to guide, as well as steer the course of her treatment.
“Within two weeks, I was already starting treatment,” she says. “Thank God we got it in time, and that I was Stage 3C and not Stage 4. It didn’t metastasize.”
She underwent six rounds of powerful chemotherapy, and her surgical oncologist introduced her to a plastic surgeon, Dr. Flores. Together, they developed her surgical treatment plan. Despite the cancer being highly treatable, and only in one breast, she opted for a double mastectomy.
“I was 100% involved in my care,” she says. “I knew the double mastectomy was not only best practice, but the best scenario for my family.”
choosing to be present
Jessica chose to do a free flap reconstruction, where natural tissue from a different part of the woman’s body is used to recreate the breasts. She thought it was a more natural option than implants, especially since implants need to be replaced every 10 years. But there was one aspect of surgery Jessica wasn’t sure about.
During mastectomy, in order to remove the breast tissue and cancerous cells, the nerves in the breast have to be severed, leaving the chest area completely numb.
“You feel nothing,” Jessica says. “The skin is just that—just skin. You feel absent. You feel not there. [So I thought] even if he’s able to reconstruct the breast, I’m not going to be able to feel it.”
a bold new technique
Dr. Flores recommended Jessica’s surgical plan include a technique called Resensation®, which gives women the possibility of regaining sensation in the breast tissue.
It’s an additional step that can be performed during reconstruction surgery that reconnects the nerves in the newly reconstructed breast with the nerves in the chest. An allograft nerve developed by Axogen is used to help bridge the gap to allow the nerve fibers to re-grow.
“I thought, You have something that’s going to make me feel better, make me happier? Give it to me,” says Jessica.
rediscovering herself
Her surgery went smoothly, but at Jessica’s one-month follow-up, she was disappointed not to have sensation back in her breasts yet. But Dr. Flores comforted her.
“He said my body wasn’t going to regenerate in just one month,” she says. “And he told me this is our journey and no matter what we’re in this together.”
The following month, Jessica realized she could sense when the nurse examined her. The a few months later, the nurse gave Jessica a little pinch to check her sensation—and to Jessica’s delight, it hurt. She yelped, bursting into tears.
“Happy tears—I knew I was going to be okay. I knew everything was going to come back to me. My journey was going to end positively.”
Jessica says her chest and breasts are where her kids slept, where they fed from. “This means nurturing to me—and [Dr. Flores] gave that back to me.”
Looking back, Jessica wants other women considering a mastectomy to know, “You need to take over your life. You need to decide what you want.”
“What is the most important to you for the rest of your life, for your journey? Because we still have years to come.”
If you’re considering a mastectomy, get in touch with a Resensation surgeon to learn more.
*The level of sensation restored following use of the Resensation technique may vary and cannot be guaranteed, due to unique anatomy and other considerations. Please consult a surgeon for more detailed information.
Resensation Articles

How does mastectomy impact the nerves in the breast?
One sometimes overlooked aspect of mastectomy is its impact on nerves. Read what happens to nerves during mastectomy and explore…
Read More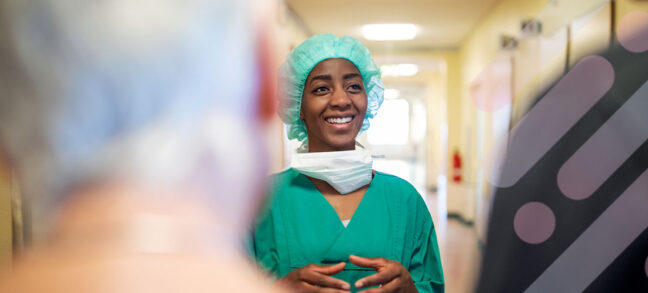
What happens during implant breast reconstruction with Resensation®?
By repairing sensory nerves, Resensation® enables you to potentially regain sensation to your chest. Read how this procedure works during…
Read More
how resensation® helped Leanna feel secure in her family’s future
With Resensation®, Leanna can be there to watch her kids grow up—without losing the feeling of being whole.
Read More
post-surgery sensory retraining: instructions and video guide
Sensory retraining is a series of exercises designed to help you reconnect with your body after breast reconstruction with Resensation®.
Read More